-
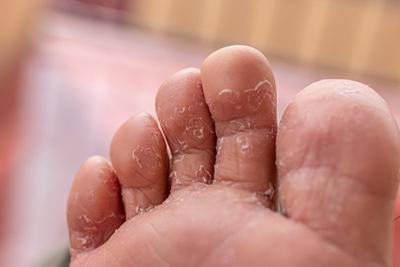
Athlete's Foot: Recognizing and Treating Fungal Infections
posted: May 01, 2024.

-
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 07, 2024.
-
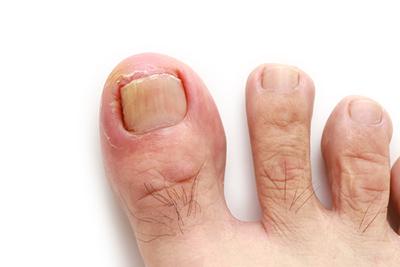
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
-
What To Expect During Heel Pain Treatment
posted: Mar. 22, 2024.
-
Treating Plantar Fasciitis
posted: Mar. 12, 2024.